I am a 48-year-old ER doctor who appears to be losing the joys in medical practice. I am not the excited person I was years before. My heart does not leap with excitement when I see cases I don’t often see. A week ago, a 29 year old woman was brought in because she had swallowed her engagement ring hidden in her dessert. Three days ago, there was a remote control lodged comfortably in a rectum. I know I would have been fascinated by it then. Not anymore. The work feels like a lull now, a schedule I need to show up to, complete, and move on from. I am unsure whether my ongoing divorce has quietly shifted something in the way I think.
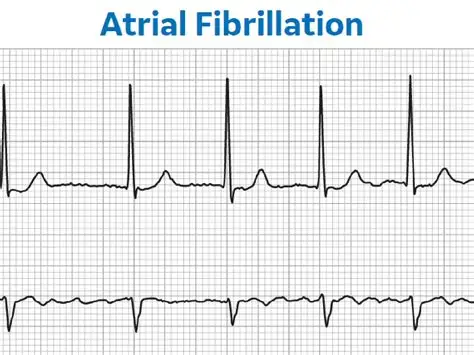
Two days ago, I saw a patient who came in with what looked like fast heartbeats. The ECG confirmed atrial fibrillation, that familiar irregular rhythm where the upper chambers of the heart stop beating in an organised way and begin to quiver instead. Speaking to him, I realised he is the main carer for three children with significant educational and emotional needs. He drinks ten to twelve cups of coffee a day just to keep himself going because he is constantly tired. I found myself respecting him for not turning to something more destructive, something that could have caused immediate havoc in his life and in the lives of the children who depend on him.
I managed him according to emergency service guidelines. I explained the diagnosis, started the appropriate medication to control the heart rate and reduce stroke risk, safety-netted him carefully, and arranged follow-up in the necessary clinic. When I asked whether he needed any additional support, he declined. He said he was managing, though some days were harder than others.
I do not know why, but I felt worse after he left. I kept thinking about what happens when “some days” becomes most days. What will he do when it gets harder than it is now? What will happen to his children if he can no longer carry everything alone?
Soon after, I saw a gentleman who had come in after a fainting episode. He admitted he had not been taking care of himself since his wife was moved into a care home. Then there was the 92-year-old man with severe mobility problems who lived alone and had no one nearby. Different illnesses, different ages, different stories, yet the same quiet thread ran through all of them. Loneliness. The kind people rarely name out loud. The kind that sits behind symptoms and slowly shapes health in ways medicine cannot easily measure.
In emergency medicine we are trained to look for the dramatic and the life-threatening. A blocked artery. A failing heart rhythm. A hidden bleed. We learn that minutes matter in stroke, that early defibrillation saves cardiac arrest patients, that sepsis can look deceptively mild before it suddenly is not. These are the facts we hold onto because they are clear and actionable. But there are other forces that shape illness more slowly. Exhaustion. Isolation. Grief. The quiet loss of purpose. They do not appear on blood tests, yet they are present in the room.
I wonder if what unsettled me most that day was not their conditions, but the mirror they quietly held up. The possibility that loneliness can arrive gradually, even in a life that once felt full.